Focus: Increased viability of donated organs
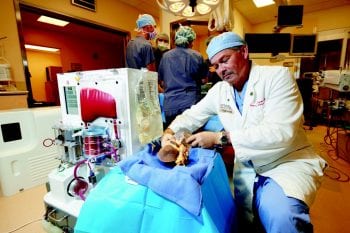
Washington University liver transplant surgeons at Barnes-Jewish Hospital historically have worked to improve a basic problem in liver transplantation: there are far too few donor organs available for patients with liver failure. A successful transplant can be life-saving for these patients, but many die while on the waiting list.
The Washington Post reported that in 2016, “7,841 livers from deceased donors were transplanted in the United States, while 14,000 people remained on the national waiting list. More than a thousand people die on the waiting list every year.”
One solution is to improve the viability of donated livers for transplant. Most recently, transplant surgeons at Barnes-Jewish Hospital are participating in a national trial comparing traditional cold storage vs. normothermic machine perfusion (NMP) for donor organs. NMP has been approved for routine use in Europe after earlier studies found it safe and feasible, but the U.S. clinical trial is ongoing. Washington University has recruited more than 25 patients to the trial and is one of the leading centers among 14 in the nation.
“While the donated liver is on the normothermic perfusion pump system, we can check parameters of function and have confidence determining whether the organ is going to work effectively, and then you can say, ‘OK, we know whether we can use it,’” says Transplant Surgery Chief William Chapman, MD, the Eugene M. Bricker Chair of Surgery.
Currently donated livers are flushed with a cold preservation solution and iced down at the time the organ is recovered. The process, however, contributes to ischemia/reperfusion injury, inflammatory damage that occurs when blood flow is interrupted until the liver is transplanted. If the organ is marginal, with more than 30 percent affected by fatty liver disease, the inflammatory damage can make it unsuitable for transplant.
Chapman led an animal study showing that NMP improved organ function in donation-after-cardiac death (DCD) livers and published findings in the journal Surgery. His research lab also has published studies on mechanisms causing liver transplant failure; most recently, a study in the American Journal of Transplantation reported that CD47 blockade reduces ischemia-reperfusion injury.
Highlights
Surgeon Adeel Khan, MD, MPH, studies disparities in access to liver transplantation. Disparities affect women, people of lower socioeconomic status and those who live a great distance from health care centers. The farther patients live from a transplant center, or if they live outside an urban area, the less likely they are to receive a transplant. When they do receive a transplant, however, there is no significant difference in surgical outcomes. Khan’s research may prove useful in helping to shape organ allocation strategies and better define geographic boundaries.
Researcher Brian Wong, PhD, is studying the role of lymphatic vessels in transplant immunobiology and organ rejection. Lymphatic vessels, which are present in donor organs but are not reconnected during the transplant procedure, re-grow after transplantation. Wong’s goal is to translate his research into novel therapeutic approaches that improve graft outcomes and prevent rejection.
Collaborative fellowship training between hepatobiliary-pancreatic and GI (HPB-GI) surgeons and transplant surgeons is proving to be a very popular component of both training programs. Section Chief William Chapman, MD, and transplant surgeons M.B. Majella Doyle, MD, MBA, and Adeel Khan, MD, MPH, treat liver and pancreas cancer along with their HPB-GI colleagues and sometimes operate together. Transplant and HPB-GI surgery fellows generally spend one to two months of the year in the other specialty. Both programs attract candidates from across the United States and globally.
